Endoscopy Staff Injury: Assessing Risks vs. Assessing Damage
by Larissa Biggers, on July 25, 2019
For years the American Medical Association has urged individuals to assess their risk for pre-diabetes; by being aware of their status or this pervasive disease, they can head off problems before they become serious. And the AMA does not stop there. It urges employers to encourage their workers to complete the health assessment, asserting that diabetes prevention is “good for business.”
Similarly, HIPPA requires its covered healthcare organizations to conduct a risk assessment. The goal is to ensure compliance and reveal areas where protected health information (PHI) might be at risk. By being proactive, entities can take action to eliminate risks for privacy violations.

Given the fact healthcare workers sustain musculoskeletal disorders (MSDs) at a rate higher than that of workers in all other industries, it would seem logical that the hospitals and healthcare facilities that employ them would want to evaluate and mitigate risks. Yet if you google “risk assessment healthcare staff” or similar phrases, results returned include “Assess Your Patients’ Risk of Falling” and “Workplace Violence Risk Assessment.” Not much is available on measuring the risks for MSDs among healthcare staff.
Do They Know?
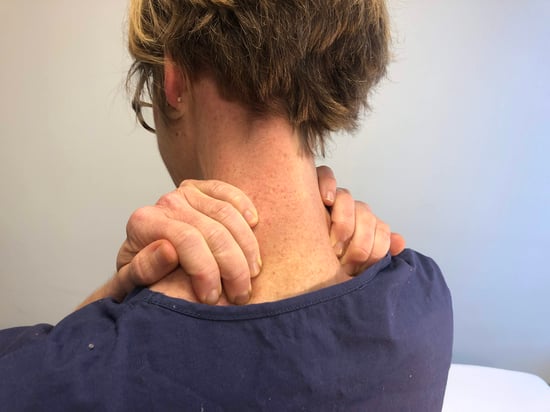
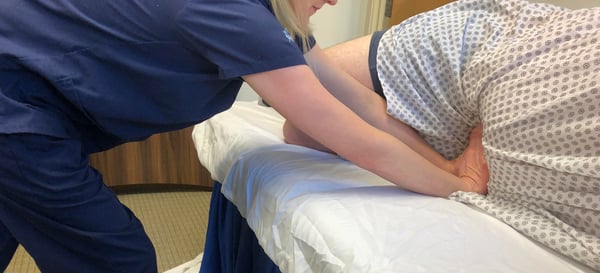
Consider the example of a busy endoscopy unit in a large hospital. A nurse or technician who assists with colonoscopies is often asked to apply manual pressure to a patient’s abdomen and / or reposition the patient as a routine part of the procedure. Given the rising rate of obesity in the US, the aging healthcare workforce, and the fact that these physical maneuvers are difficult under the best of conditions, injury seems inevitable. Indeed, one in two endoscopy nurses has suffered a work-related injury. But because these demands are part of the job, many workers fail to report injuries and instead suffer in silence. Some hospitals might not realize the severity of the problem and might not think that there is anything to assess.
Do They Care?
Annually, hospitals pay an estimated $6.2 billion and lose at least 926,000 work days due to job-related injures. Furthermore, a 2018 study reveals that 43% of healthcare executives believe staff shortages are worse now than in the previous year. Based on these facts alone, it would seem logical that hospitals would want to retain staff by ensuring their safety, at a minimum. But many healthcare organization believe that the costs of establishing injury prevention programs, i.e., Safe Patient Handling and Mobility (SPHM) programs, are prohibitive and so choose to do nothing.
Spending Wisely
If a hospital purchases equipment that does not meet the needs of its staff, it is unlikely to see a reduction in injuries or a return on investment. This type of mistake can be avoided with a simple assessment. For instance, if an endoscopy unit discovers that 50% of its staff experience hand pain after assisting with colonoscopies, it can address that specific issue with the appropriate SPHM equipment and training, as opposed to investing in expensive, but unnecessary tools.
If it is acquired strategically, SPHM equipment pays for itself quickly. The Veteran's Health Administration, for example, found that implementing SPHM programs with appropriate equipment mitigates risks to employees. Specifically, doing so reduced manual patient handling injuries by 40% between 2006 and 2014 in their facilities.
A Proactive Approach: Risk Assessment Tools
- OSHA‘s tool for hospital managers (How Safe Is Your Hospital for Workers: A Self-Assessment) determines a facility’s risk for employee injury. It focuses specifically on injury incidence rate, lost work days, costs, and current safety programs.
- ColoWrap's GI / Endoscopy Unit Risk Assessment determines the likelihood for injury among endoscopy staff. It not only explores tasks performed by staff but also looks at characteristics of the patient population.
After the Fact: Injury Assessments
- The Patient-Specific Functional Scale (PSFS) asks individuals to identify and rate activities that they cannot perform or can only perform with difficulty and measures the severity of an injury before and after intervention.
- Disabilities of the Arm, Shoulder and Hand (DASH) is a questionnaire that assesses an individual’s ability perform certain activities involving the arms, shoulders, and hands.
If injury risk assessments were obligatory, the need for injury evaluations would be minimal, but here's the reality; 76% of nurses experience physical discomfort at work, and 12% were injured on the job in the past year. Rather than reacting after the fact, healthcare entities should take care of their employees before they are injured. Although challenging, the task is not impossible.
One reason for optimism is that more and more nursing students are being taught to advocate for their safety. One nursing school instructor explains, “Our culture is that if they go to work somewhere that doesn’t have the equipment, they should be asking, for safety reasons, why not? They should be assertive and speak up so the facility can really look into this.”



