5 Indirect Costs of Endoscopy Staff Injury: #1 Presenteeism
by Larissa Biggers, on May 17, 2019
This blog series explores five indirect costs stemming from endoscopy staff injury and their real-life implications on GI units. Installment #1 covers presenteeism, which occurs when an employee is physically at work but because of pain, injury, illness, or other medical conditions, is not performing adequately.
A GI nurse addresses the impacts of injury
“[Most] of the time… [injured staff] are placed in another department to work while they are going through therapy, usually some sort of desk job. So we shuffle the remaining deck and sincerely hope there are enough bodies to continue to function, and hope usually withers to begging people to work extra shifts. [When] an employee is allowed to work modified light duty within our department, it has placed an undue burden on the team as they get intermittently pulled from whatever duties they were assigned to "pop in" when the modified employee cannot perform some particular task: transferring a patient, lifting something, etc. There is no one to cover the helper; they have to drop what they're doing and go. Staff get frustrated; doctors don't want to be abandoned; the injured worker feels embarrassed; and the patients watch, all of which is obviously not ideal, nor is it always possible. Best to avoid the injury in the first place!”
The direct costs of endoscopy staff injury are typically easy to understand and measure. They include doctor visits, medical bills, medicines, and rehabilitation. But direct costs are just the tip of the iceberg. Indirect costs, those below the surface, comprise the unbudgeted expenses required to get the employee back to pre-injury status—or to replace that employee.
 Direct costs: what you see; indirect costs: what you get
Direct costs: what you see; indirect costs: what you get
Soft costs of of presenteeism
Presenteeism is difficult to address in part because it is often hidden. It’s obvious when a colleague does not show up for work, but you can’t always tell when—or to what extent—physical problems are affecting an employee’s performance. If they look okay and don’t complain, it’s hard to know that they are suffering.

Nurses, perhaps because they are often trained to put patients before themselves, are particularly prone to presenteeism. Seventy-one percent of respondents to an American Journal of Nursing survey reported experiencing musculoskeletal pain; and 62% scored at least a 1 on a presenteeism scale of 0 to 10, indicating that health problems had affected work productivity at least "a little." Presenteeism was significantly associated with a higher number of patient falls and medication errors and lower quality-of-care scores.
Consider this example:
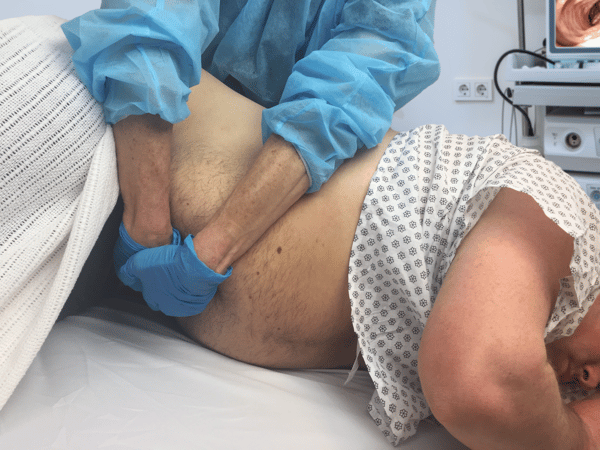
Bobbi, an endoscopy technician, has had nagging pain in her right hand for the past six months. It gets worse when she applies abdominal pressure to obese patients. She could call in sick but is saving her days off for when she is really ill. Plus, she does not want to let the rest of her team down.
Even though Bobbi does not want to burden her colleagues, she is doing just that. When people don’t feel well, they simply cannot do their best work, and that has an impact on the entire team.
- Bobbi’s pain affects the quantity of work she can perform. During colonoscopy she cannot hold abdominal pressure for more than 30 seconds at a time, when she has to ask for help or take a break. This can make cases longer (requiring additional sedation for patients), frustrates physicians, and increases the workload for the nurse in her procedure room.
- It affects the quality of her work. Bobbi dislikes working with overweight or obese patients because she knows how physically difficult patient-handling tasks can be with this population. As a result, she is less engaged with them, and the unit’s patient satisfaction scores have suffered over the last four to five months.
The measurable financial impact of injury
Indirect costs related to presenteeism have long been invisible to employers. Taken as a whole, though, it appears to be a more expensive than absenteeism. Numerous studies show that presenteeism costs employers two to three times more than direct medical care, and some estimates indicate that presenteeism accounts for 75 percent of productivity loss. Two recent articles in the Journal of the American Medical Association reported that pain conditions such as arthritis, headaches, and back problems cost employers nearly $47 billion a year in reduced performance at work.
While these statistics are applicable the US workforce in general, data is similar for healthcare specifically. A four-year review of presenteeism data among employees of a large healthcare system found that two of the five conditions that cost the system at least $1 million annually are common among endoscopy staff; chronic back pain accounted for an estimated $1.21 million each year in presenteeism costs. For arthritis the estimate was $1.04 million annually. Incidentally, chronic back pain led to a daily productivity loss per person of 16.7 minutes, and arthritis caused an 8.2-minute decrease.
Presenteeism and change
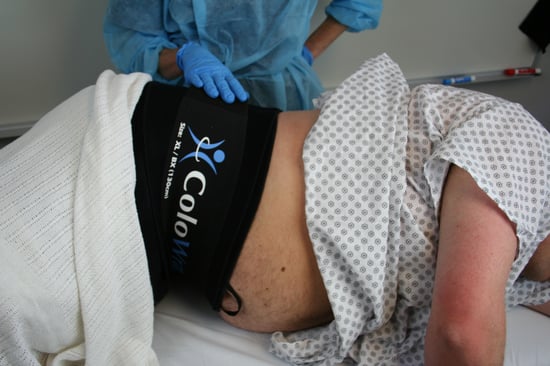
The indirect costs of presenteeism have been notoriously difficult to prove, but recently, a few companies have begun measuring the prevalence of illnesses and medical problems that compromise job performance, calculating the related productivity loss, and investing in solutions that truly diminish that loss. For instance, for endoscopy staff, a device that mitigates the need for applying abdominal pressure or repositioning patients would be well worth the the investment, even if it prevented just one injury per year.
In contrast, trying to reduce a GI unit’s direct costs by cutting benefits would result in false savings that would be offset by the indirect cost of reduced productivity (not to mention the direct costs associated with paying for an injury). Healthcare systems and other employers must take into account presenteeism data when implementing programs to combat low productivity. Protecting employees' health can result in reduced presenteeism, which can increase profits. Plus, it's the right thing to do.


