The Microbiome: Beyond Gut Health
by Larissa Biggers, on February 08, 2019
The human gut microbiome comprises all of the bacteria in in the human intestine, which amounts to over 100 billion bacteria. This outnumbers the cells in our bodies 10 to 1. Although probiotic products touting gut health are currently flooding the marketplace (ranging from dietary supplements to cake mixes), there is no consensus on what a healthy human microbiome looks like, and none of these products have been approved by the FDA to treat or prevent specific diseases. While most agree that it is essential to human health, facts about the microbiome and how it functions in the body are still under investigation.
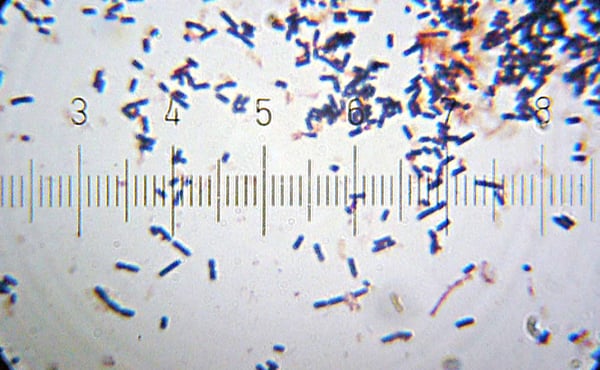
Lactobacillus Acidophilus
The microbiome as a diagnostic tool
The microbiome might prove to be an important tool for diagnosing colorectal cancer (CRC). One study found that when microbiome data was considered along with known risk factors, the ability to predict precancerous adenomatous polyps increased by a factor of 4.5, and there was a 5.4-fold improvement in forecasting invasive CRC. Researchers also determined that gut microbiome signatures (the composition of an individual’s gut microbiota) were better than fecal occult blood testing in differentiating patients with precancerous adenomatous polyps from those with invasive colorectal cancer. While these findings could shape adjunct testing for CRC in the future, integrating gut microbiome data into routine screening requires faster and more affordable bacterial assays.
A factor in CRC
Fortunately, a perfect understanding of the microbiome is not required to undertake clinical interventions. Recently, the Dana-Farber Cancer Institute received up to $25 million to investigate how certain microbes contribute to the development CRC and how they affect patient response to treatment. As part of the project, the Institute will seek to determine the difference between a healthy microbiome and one associated with cancer. Furthermore, it will uncover ways to manipulate the microbiome to help prevent and treat cancer.
Already, studies have found that restoring function to the microbiome can prove beneficial for preventing cancer and improving the effectiveness and safety of cancer treatment. For instance, administering certain Lactobacillus and Bifidobacterium strains is associated with biochemical and histologic changes that might decrease the risk of developing malignancy. On the flip side, animal studies have shown that bacteria can contribute to CRC through a direct interaction with the immune system, production of metabolites associated with cancer, and release of genotoxic factors that induce disease. This research also identified organisms that might influence CRC development.
Looking ahead
Ultimately, microbiome diagnostics could be a routine part of clinical care and individualized interventions such as probiotic administration aimed at reducing CRC risk. Before that that can happen, additional clinical research is required to, among other things, determine probiotic therapy regimens that result in a reproducible clinical benefit.


