Women Gastroenterologists: Underpaid, Under-Represented
by Larissa Biggers, on March 07, 2019
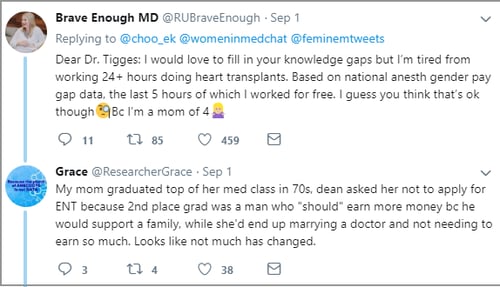
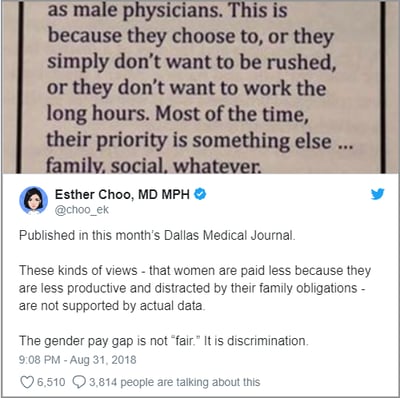
Happy International Women's Day (March 8)! Today is a global celebration of the achievements of women. It also marks a call to action for accelerating gender parity. ColoWrap wants to honor the accomplishments of female gastroenterologists AND highlight gender disparities that are narrowing but are not yet resolved. We are sharing an updated version of a 2018 post to reignite the conversation.In the fall of 2018, a physician’s response to a Dallas Medical Journal survey evoked angry retorts and fueled discussion about inequities between male and female physicians. Dallas County Medical Society members were asked if there was a pay gap between male and female physicians, and if so, how it could be remedied.
Dr. Gary Tigges replied that female physicians choose to not work as hard or see as many patients as men, and as a result are (justifiably) paid less. Furthermore, he noted that nothing needs to be “done” about the situation.

Some say his remarks were taken out of context. Others claim that they are indicative of a discriminatory, sexist climate in medicine. No matter your position, the fact remains that there is a disparity between male and female physicians, and not just a financial one.
Facts Are Facts
According to the latest Doximity Physician Compensation Report, female physicians earn an average of 27.7% less less than their male colleagues. In fact, in no medical specialty do they make more than men. The report also indicated that female gastroenterologists (GIs) earn approximately 19% less than their male counterparts. The results of Medscape's 2018 Gastroenterologist Compensation Report were even more dramatic, with an average disparity of 28%.
According to Dr. Tigges, because women elect to work less, the salary gap is “fair.” Yet even after adjusting for factors like lack of seniority, work hours, maternity leave, and geographic region, female GIs earn only 75% to 80% of what men are paid. The data simply do not support his assertion.
More Than a Pay Gap
Not only are female GIs at a financial disadvantage compared to men, there are fewer of them. Although approximately 50% of medical school students and 40% to 50% of third-year internal medicine residents are women, only 25% to 30% of GI fellows and 13% of GIs in the U.S. are female.
Ironically, though, studies show that female patients strongly prefer female GIs for both office visits and colonoscopies. Furthermore, in terms of effective colonoscopies, female endoscopists have a higher adenoma detection rate. After adjusting for patients' age, sex, and colonoscopy indication, they were found to have approximately 26% greater odds of detecting an adenoma than did men.
So why are there so few women GIs? Some hypothesize that because specialties like gastroenterology and cardiology require significant on-call duties, women, who often bear the brunt of responsibility for childcare, are less attracted to these specialties. Yet, 85% of OB-GYNs (who are on call for many more hours than GIs) are women.
Leadership Positions
Similar numbers are reflected in academia and professional societies. A 2016 survey of the top 50 NIH-funded medical schools found that only 13% of department leaders were women. Until 2017, the American College of Gastroenterology (ACG) had just two female presidents, and the American Gastroenterological Association (AGA) elected its first female president in 1942 and 1943; the next was in 2010.
Baby Steps
Grace Elta, co-author of “Is the glass ceiling in gastroenterology gone?” believes that the tide could be turning. In an interview published in ACG Update, she stated, “The numbers [of women in GI] are clearly increasing. It’s slow, but everything in medicine is slow. I guess it’s surprising to me how slow…. It’s already been over 20 years where medical schools have been around 50% women. You think, ‘Wow, it’s been that long. Why is it taking so long for GI and cardiology to catch up?’ But they are catching up. I think it is happening, it’s just slow. I think role models help, seeing that other women have done it. I think mentors help, having someone to talk to, to say ‘You can do this.’ I think that makes a big difference.”
Elta points to another encouraging sign, committee membership in national societies. In 2011 through 2014, the proportion of requests for committee appointments from women (16% to 21%) was higher than the proportion of female membership in GI societies. In addition, those numbers remained consistent throughout that period. But while committee membership might be a step in the right direction, it is a far cry from gender equity in GI.
Larger Strides
While many individuals, both men and women, were outraged by Dr. Tigges’ remarks, he did get one fact right—the pay gap exists. Elta herself notes that while there may be progress in other areas, one that needs attention is salary equity. In contrast to Tigges, she states that the discrepancy is “grossly unfair and likely will not change until greater transparency occurs around salaries.” The American Medical Association (AMA) agrees. It has pledged to close the pay gap and take steps to advance gender equity. Plans include: advocating for pay structures based on objective, gender-neutral criteria; creating educational programs on equitable compensation negotiation; launching an awareness campaign on doctors’ rights under the Lilly Ledbetter Fair Pay Act and Equal Pay Act; and hosting workshops on the role medical societies can play in advancing women in their fields.
And there are other positive signs; In 2017, the presidents of the four large national GI societies were women. And the Medscape survey indicated that 75% of female GIs are seeking promotion, compared to 39% of men.
These are all harbingers of progress. May the momentum continue in 2019.


